Tip of the Week
Interpreting: The Fine Points of Empathy
 Here’s a concise piece on one of the subtle aspects of interpretation — What does compassion mean for medical interpreters? — offered by Yuliya Speroff on the Medical Interpreter Blog.
Here’s a concise piece on one of the subtle aspects of interpretation — What does compassion mean for medical interpreters? — offered by Yuliya Speroff on the Medical Interpreter Blog.
In her piece, Speroff has tips on communicating a greater sense of empathy and compassion by harnessing strategies that include:
- Active listening and being present,
- Conveying all nuances of a message, including the emotional underlayment,
- Displaying cultural sensitivity and facilitating dialogue when cultural nuances affect understanding.
June 22 Is Twin Cities World Refugee Day!
Above: scenes from last year’s event.
Join CAPI USA for its annual celebration on Twin Cities World Refugee Day, scheduled for Centennial Park in Brooklyn Center, 10:30 – 5 pm on Saturday, June 22. There’s free live entertainment, food and vendors from around the world, children’s activities, a community resource fair, and interactive displays.
Location: Centennial Park, 6301 Shingle Creek Pkwy., Brooklyn Center, MN 55430
View CAPI’s website for more details on this event.
|
|
Helping LGBTQ+ Newcomers Fit In
 Here’s a free webinar offered by the resettlement specialists, Switchboard, designed to help newcomers succeed in their changed environment. The webinar is set for noon to 1:15, Tuesday, June 25. The target audience is direct service providers, managers, and others in refugee resettlement who, organizers say, “want to cultivate spaces where LGBTQ+ newcomers feel embraced, valued, and respected.”
Here’s a free webinar offered by the resettlement specialists, Switchboard, designed to help newcomers succeed in their changed environment. The webinar is set for noon to 1:15, Tuesday, June 25. The target audience is direct service providers, managers, and others in refugee resettlement who, organizers say, “want to cultivate spaces where LGBTQ+ newcomers feel embraced, valued, and respected.”
Among the take aways: You’ll —
- Learn how to examine the cultural and interpersonal dynamics of welcoming LGBTQ+ newcomers
- Learn best practices for communication strategies, confidentiality considerations, and the nuances of belonging for LGBTQ+ newcomers within their families, ethnic communities, and new local communities.
Natural vs. Artificial Intelligence: Some Pushback
 In his recent essay, The Dehumanization of the Healthcare Interpreter, Or How I Learned to Love Natural Intelligence, Fleuncy Inc. President Bill Glasser seemingly accepts that medical interpretation, driven by artificial intelligence, will inevitably dominate in the healthcare environment. His analysis dwells on what will be lost in the transition.”
In his recent essay, The Dehumanization of the Healthcare Interpreter, Or How I Learned to Love Natural Intelligence, Fleuncy Inc. President Bill Glasser seemingly accepts that medical interpretation, driven by artificial intelligence, will inevitably dominate in the healthcare environment. His analysis dwells on what will be lost in the transition.”
“As I watch and presume that Generative AI and Large Language Models will take over for the face-to-face human interpreter in the room,” Glasser writes, “it strikes me that we may have forgotten how caring for sick people works.” He makes a case for the healing powers of a human touch that for now is not replaced by a machine.
Psych First Aid for Crisis and Trauma
 Get free virtual classes on psychological first aid to support people after public emergencies, disasters or personal crisis and trauma. Presented by M Health Fairview Community Advancement, the two hour training is designed for community members and health care professionals, and is available in Spanish and English.
Get free virtual classes on psychological first aid to support people after public emergencies, disasters or personal crisis and trauma. Presented by M Health Fairview Community Advancement, the two hour training is designed for community members and health care professionals, and is available in Spanish and English.
The Spanish session is offered from 9 -11 am, Wednesday, June 5. Register here.
Th English version is from noon – 2 pm, Thursday, June 13. Register here.
Get more information by contacting Kathryn.taylor@fairview.org.
Your Native Language: Can You Lose It?
Then as an adult in 2020 she moved to Paris full time to run The Dial, a magazine she founded to bring more local journalists and writers to an English-speaking audience.
That’s where some trouble started. A more fluent friend observed that Schwartz’s attempt to translate English speech forms into French missed subtle points. She was, her friend noted, effectively shouting at others.
Locutions that would seem bizarre in English were expected in French. “Compared with English, French is slower, more formal, less direct,” Schwartz explains. “The language requires a kind of politeness that, translated literally, sounds subservient, even passive-aggressive. I started collecting the stock phrases that I needed to indicate polite interaction. “I would entreat you, dear Madam …” “Please accept, dear sir, the assurances of my highest esteem.”
You can read much more regarding this treacherous path in the New York Times article, “Can You Lose Your Native Tongue?”
The piece continues to examine how for the bilingual, languages are at a sort of war with each other to determine dominance. It’s an eye-opening look at how the many immigrant language learners must struggle with expressing themselves as they sort through the various languages in their heads.
Get Square with Language Access Regs
 Do you have questions about your organization’s legal requirements to guarantee language access for patients and clients with limited English?
Do you have questions about your organization’s legal requirements to guarantee language access for patients and clients with limited English?
Then check out this issue brief from the National Health Law Program on Title VI of the Civil Rights Act of 1964. This clearly written piece lays out the details of the recently finalized regulations from the Office for Civil Rights for providers and policy makers.
The Immigrant View on Running for Office
 Sahan Journal delivers again with a piece on the life circumstances that led Anquam Mahamoud to run for a Minnesota House seat in the south Minneapolis district 62B.
Sahan Journal delivers again with a piece on the life circumstances that led Anquam Mahamoud to run for a Minnesota House seat in the south Minneapolis district 62B.
Mahamoud was born in San Diego but moved to Minneapolis with her family in 1998 in a search for a lower cost of living and better education. With her mother working more than full time, Mahamoud took on the duties of managing the household and caring for her three brothers.
She started working at 15, for a $5.15 per hour wage, which she contributed to groceries, clothes and supplies for her siblings. Her realization: “No child should have to sacrifice their childhood to support their family financially.”
Having graduated from St. Catherine, she now works at a substance treatment center and mental health facility. Her core issue is access to health care. Mahamoud says her life experiences have turned her attention to the necessity for reliable insurance. “I strongly advocate for accessible universal health care, believing that the government can take steps to ensure everyone has the health care they need.”
The Sahan Journal story, Get to know Anquam Mahamoud, the House 62B hopeful who puts health care front and center, provides an interesting perspective on the forces that drive recent immigrants into the political process.
Translated Help in Explaining Hospice and Palliative Care
 If you follow the work of the Minnesota state legislature, you noticed the recent commotion over medical assistance in dying — a legislative effort to offer medical help to terminally ill people in ending their lives. The legislation appears to be going nowhere this year, but it did result in an airing of the options in Minnesota currently available to those with painful conditions that sap them of their desire to live.
If you follow the work of the Minnesota state legislature, you noticed the recent commotion over medical assistance in dying — a legislative effort to offer medical help to terminally ill people in ending their lives. The legislation appears to be going nowhere this year, but it did result in an airing of the options in Minnesota currently available to those with painful conditions that sap them of their desire to live.
The business of dying can be especially confounding for those with limited English and various cultural assumptions. For a series of translated materials that explain hospice and palliative care in Hmong, Spanish and Somali, take a look at resources compiled by the Minnesota Network of Hospice and Palliative Care. The group seeks to raise awareness about cultural values that surround caring for those nearing the end of their lives.
Among the topics:
- Three Components of Hospice Care
- Advance Care Planning
- Portable Medical Orders
- Hospice Care FAQ
- Palliative Care in Minnesota FAQ
- Choosing Hospice Consumer Guide
Find these translated print materials here.
Interpret This: A Dying Dialect Linked to Ancient Greek
On one hand, you’ve got the dominant languages of the world, which include English with 1.4 billion speakers, Mandarin with 1.3 billion speakers and Hindi with 602 million speakers. And then there is Romeyka.
Romeyka is an endangered form of Greek preserved in remote mountain villages of northern Turkey. Now spoken by only a few thousand people, it’s described by researchers as a bridge to the ancient world, sharing more with the language of Homer than with modern Greek. (Listen to a comparison in the video above.) With no written form, it has lingered on orally in an area around the Black Sea coast.
With Romeyka speakers aging, and younger people not exactly clamoring to learn the aged tongue, it’s another language in danger of disappearing from the world.
In this story from the Guardian, Endangered Greek dialect is ‘living bridge’ to ancient world, you can get a look at the current effort to preserve Romeyka. But the piece also includes this bit of perspective from University of Cambridge historical language professor Ioanna Sitaridou. “Obviously I love all languages and I would like to see them preserved,” she says. “But I’m not one of these people who think languages have to be preserved at all costs. And at the end of the day, it’s not exactly down to me. If the speakers decide to pass it on, great. If the speakers choose not to pass it on, it’s their choice.”
Your Portal: Is It a Barrier?
 Here’s another wrinkle in the attempt to communicate effectively with LEP patients: is your patient portal truly accessible? With growing use and dependence on web-based portals, are all patients getting an even shake?
Here’s another wrinkle in the attempt to communicate effectively with LEP patients: is your patient portal truly accessible? With growing use and dependence on web-based portals, are all patients getting an even shake?
According to Intersect: A Newsletter about Interpreting, Language and Culture, this is a communication sector that could use more examination. Last year about a third of immigrants reported “obstacles in receiving respectful communication from their providers.”
Among those obstacles: the patient portal that has become “the de facto channel for engaging patients in their care outside of facilities.” Use of these portals is less among Black and Hispanic patients compared to their white peers.
The Hidden Burden for Child Interpreters
 It’s not news to observe that children often end up serving as interpreters and translators for family members with limited command of English. But recently University of California researchers delved into a largely unexplored area regarding the complicated intersection of words, body language and facial expressions that children are being asked to simultaneously process and communicate to their elders.
It’s not news to observe that children often end up serving as interpreters and translators for family members with limited command of English. But recently University of California researchers delved into a largely unexplored area regarding the complicated intersection of words, body language and facial expressions that children are being asked to simultaneously process and communicate to their elders.
The result: kids are left to grapple with situations that they don’t expect, or dimly understand themselves. Observes UC researcher Sivenesi Subramoney, children are often proud of their role and responsibility, but “they aren’t nearly as prepared to interpret the unspoken. Emotion brokering catches them off guard and can lead to escalation, frustration or embarrassment.”
Read more about what Subramoney calls “emotion brokering” here.
Getting the Joke in ASL
 When Sam Corbin, the crosswords editor for the New York Times, took on the project of learning ASL, she couldn’t resist the temptation to do what she routinely did with spoken and written English: play around with words. Being something of a joker herself with a deep attraction to unleashing a pun, she became fascinated by how hand movements translate into humor.
When Sam Corbin, the crosswords editor for the New York Times, took on the project of learning ASL, she couldn’t resist the temptation to do what she routinely did with spoken and written English: play around with words. Being something of a joker herself with a deep attraction to unleashing a pun, she became fascinated by how hand movements translate into humor.
“Like hundreds of other signed languages spoken around the globe,” she writes, “ASL expresses meaning through a combination of hand shapes and movements, palm orientations, use of space around the body and nonmanual signals such as facial expressions and lip movements. While in English, a given word’s definition tends to dictate its usage, each of ASL’s meaning-making elements convey definitions. Some signs may begin as one word but transform into a question with a shift of the eyebrows — or, with a different hand movement, become a clever turn of phrase.”
Read the complete article: American Sign Language Reveals Wordplay Beyond Sound — In a visual language, a subtle hand movement can help you get the joke.
Newly Arrived: The Ecuadorians
 The excellent online news outlet, Sahan Journal, recently offered a deep look at Minnesota’s surging Ecuadorian immigrant population in this piece, Ecuadorians fleeing violence and economic distress seek a new start in Minnesota. While fewer than 200 Ecuadorian emigres arrived here in 2019, the number grew to nearly 2000 in a portion of 2024. It’s a 900 percent jump in just five years.
The excellent online news outlet, Sahan Journal, recently offered a deep look at Minnesota’s surging Ecuadorian immigrant population in this piece, Ecuadorians fleeing violence and economic distress seek a new start in Minnesota. While fewer than 200 Ecuadorian emigres arrived here in 2019, the number grew to nearly 2000 in a portion of 2024. It’s a 900 percent jump in just five years.
The Sahan Journal piece, as part of its ongoing census data reporting, examines the data and resources available to the newly arrived. It provides a look at conditions within Ecuador that drive people to traverse the dangerous Darien gap on their journey to escape violence and poverty at home. The story also hits positive notes of the efforts of Ecuadorians here to build businesses and support groups as they make the transition to a new life.
This is just another example of why it’s worth keeping a close eye on Sahan Journal for its perspective on immigrant life here, written from the point of view of those experiencing it.
(In case you thought the trip through the Darien gap as an interesting stroll, check out this documentary video that reveals it for a mud-clogged, gang-run shakedown operation for desperate people already living on the edge.)
AI and Language Services: A Take on the Future
 Like most everyone else involved in language service, you’re probably hearing footsteps from artificial intelligence interpretation and translation tools and wonder how they may alter your work. For a look at the current state of AI in translation, and related near-future issues, download this report, Current Usage, Sentiment,and Future Expectations of AI Among Language Service Providers and Remote Interpreters, from the firm boostlingo.
Like most everyone else involved in language service, you’re probably hearing footsteps from artificial intelligence interpretation and translation tools and wonder how they may alter your work. For a look at the current state of AI in translation, and related near-future issues, download this report, Current Usage, Sentiment,and Future Expectations of AI Among Language Service Providers and Remote Interpreters, from the firm boostlingo.
Among the pros of AI assistance noted in the report:
- quickly identify and provide new terms during live interpretation sessions
- clarify spoken content when clients/patients have heavy accents or use slang expressions
- search quickly for appropriate medical terms.
And a few of the cons:
- sometimes questionable accuracy
- the need for careful post-processing checks
- the learning curve can slow down productivity at first
- providers don’t trust it as a replacement and see AI use as complementary to human expertise.
The bottom line:
The blend of human expertise and AI capabilities can result in hybrid models where AI handles volume and speed, while humans ensure quality and cultural relevance… By positioning AI as a supportive tool rather than a replacement, the industry can harness its potential without sidelining human professionals.
For Non-Muslims: A Ramadan Etiquette Guide
 With Ramadan underway from now through April 9, this is the time to brush up on related good manners when interacting with Muslim co-workers and friends. Ramadan is the ninth month of the Islamic lunar calendar, during with which the faithful fast from sunrise to sunset.
With Ramadan underway from now through April 9, this is the time to brush up on related good manners when interacting with Muslim co-workers and friends. Ramadan is the ninth month of the Islamic lunar calendar, during with which the faithful fast from sunrise to sunset.
For a list of top ten tips on avoiding boorish behavior, see this CNN piece by , A Ramadan etiquette guide for non-Muslims.
“You don’t have to fast with us…,” Ahmed observes. “…but try not to schedule a work lunch.”
For a more personal and local look at the challenges and enriching aspects of Ramadan, check out this reprint from MinnPost by Ahmed Tharwat, Ramadan — a personal reflection.
The Fight to Preserve Threatened Languages
 For an close look at the causes and effects of language diversity in an urban area, check out this new book, Language City: The Fight to Preserve Endangered Mother Tongues in New York, by Ross Perlin
For an close look at the causes and effects of language diversity in an urban area, check out this new book, Language City: The Fight to Preserve Endangered Mother Tongues in New York, by Ross Perlin
Perlin observes that up to half of the world’s 7,000 languages are likely to die over the next few centuries. But the book isn’t a sob-story for threatened languages so much as collection of case studies on how displaced people rebuild their lives in a place where half the residents speak a language other than English at home.
A New York Times Book Review has this to say about Language City; “Throughout Perlin never misses the chance to reinforce a key point: The history of New York’s lesser-known languages is also that of the traumas of many speakers. Some fled genocide (as in the cases of Western Armenian and Judeo-Greek), others mass deportation (languages of the North Caucuses), racial violence (Gullah, an English-based Creole) or starvation (Irish). Linguistic minorities “have been overrepresented in diaspora,” Perlin points out, because they are “hit hardest by conflict, catastrophe and privation and thus impelled to leave.”
The Gold Standard: Care in the Language of Patients Being Served
 What’s the health impact when kids from minority or indigenous-language-speaking families get care that is not in their native tongue? According to Harvard Medical School researcher Ann Miller (right), there’s an 11 percent difference between them and native speakers in key early childhood development measures.
What’s the health impact when kids from minority or indigenous-language-speaking families get care that is not in their native tongue? According to Harvard Medical School researcher Ann Miller (right), there’s an 11 percent difference between them and native speakers in key early childhood development measures.
So what’s going on here? The trouble isn’t that speaking an Indigenous or minority language is the cause of developmental delays, Miller argues. The real reason is discrimination and lack of equitable access to health care and education for children and families in their home languages.
“The gold standard of health care, education, and child development services,” she says, “should be to deliver care in the language of the people you’re serving.”
Tune in to Immigrant Kids with Serious Medical Conditions
 Find out more about how to better serve immigrant families that include children with significant medical conditions during this 11 am, Monday, February 26 webinar sponsored by Switchboard.
Find out more about how to better serve immigrant families that include children with significant medical conditions during this 11 am, Monday, February 26 webinar sponsored by Switchboard.
About 10–15 percent of refugee children have significant medical conditions, and their needs differ from those of adults. Presenters will address unique considerations for serving newcomer children, including
- the intersection of multiple medical diagnoses,
- supporting children’s families,
- and communicating across the migration continuum
Speakers include Elizabeth Dawson-Hahn, MD, MPH, an attending physician at Harborview Medical Center in Seattle, where she co-leads the Refugee Health Promotion Project, caring for medically complex refugee children shortly after arrival.
Register to learn more about significant medical conditions.
|
|
Tragedy Upon Tragedy: A Family’s Interpreter, Slain
 Peter Wang served in a familiar role for his Florida family. His parents, who had been smuggled into the United States from Fujian, a province in southern China, in the late 1990s, arrived without knowing English. They worked in restaurant jobs, managing eventually to buy a restaurant of their own. Despite several efforts to learn English, they eventually gave up.
Peter Wang served in a familiar role for his Florida family. His parents, who had been smuggled into the United States from Fujian, a province in southern China, in the late 1990s, arrived without knowing English. They worked in restaurant jobs, managing eventually to buy a restaurant of their own. Despite several efforts to learn English, they eventually gave up.
Their link to the larger world was their son, Peter, who translated school notes, doctor’s appointments, and all the other interactions that required a command of English. But that link was sundered when Peter was among the victims of the Stoneman Douglas high school shooting in Parkland, Florida.
For a sensitive and heart-breaking account of his family’s effort to contend with grief and reorganize the mundane details of life with little command of the language, see this New York Times piece, Lost at Parkland: ‘Peter Was Always My Translator’. It’s another, complicated look at the difficulties of contending with life in the United States with limited English ability.
Substance Abuse in Refugee, Immigrant Communities: Learn More
 Get the low-down on substance abuse issues in refugee and immigrant communities at the Tuesday, February 13 meeting of the Minnesota Immigrant and Refugee Health Network. Set for 9:30 to 11 am, this online and phone session will bring you information on resources and connections to help you prevent substance abuse, plus support those who are in need of intervention.
Get the low-down on substance abuse issues in refugee and immigrant communities at the Tuesday, February 13 meeting of the Minnesota Immigrant and Refugee Health Network. Set for 9:30 to 11 am, this online and phone session will bring you information on resources and connections to help you prevent substance abuse, plus support those who are in need of intervention.
Presenters from the Karen Chemical Dependency Program and Alliance Wellness Center will lead this interactive event. Bring updates and insights to share from your work in the field.
Register for the MIRHN meeting before the morning of the meeting. You’ll receive instructions on how to join the session online or by phone. Questions? Email cynthia.trevino@state.mn.us
Interpreters: Get YouTubed
Fall down a rabbit hole of videos on practice and training for medical interpreters at this YouTube channel, Interpret Your World. You’ll find dozens of short videos on subjects such as allergies, ashtma, chest pain, COPD and much more, plus interactive interpreting scenarios. Organizers promise you’ll “enhance your interpreting prowess by engaging with our exclusive YouTube channel tailored to cater to the needs of interpreters and translators across diverse levels and languages. Find out for yourself here.
For Refugee Community Outreach Workers: Safety Tips

Dawn Higgins
The world of commotion that drives refugees from their homes sometimes spills over into their new home here, with distress and tensions that can have an impact on community sponsors, volunteers and resettlement office staff. Here’s a webinar on basic safety and situational awareness for those working in communities of newcomers.
Safety guidance will be offered by Church World Service Director for Security Dawn Higgins at this free January 29 session starting at 11 AM. Register here for the safety training.
Get Help Creating a Language Access Plan
 Time to update your organization’s language access plan to serve clients better, and to meet the dictates of state and federal law? Here’s help from Multilingual, which has drafted a concise summary — How to Create a Realistic Language Access Plan.
Time to update your organization’s language access plan to serve clients better, and to meet the dictates of state and federal law? Here’s help from Multilingual, which has drafted a concise summary — How to Create a Realistic Language Access Plan.
This combination podcast and web page lays out key facts about consumers’ legal rights, and what to consider when putting together a language access plan. It’s a quick look at the basic questions you should answer when considering how to serve limited English speakers more effectively.
A well thought out plan isn’t just a set of guidelines, the authors note. “It’s also a living testament to your dedication to serve all customers.”
A Surge in Afghan Refugees
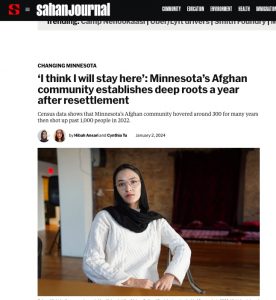 The excellent Sahan Journal reports a recent three-fold increase in Afghan refugees landing in Minnesota, and states that even that is an underestimate.
The excellent Sahan Journal reports a recent three-fold increase in Afghan refugees landing in Minnesota, and states that even that is an underestimate.
According to the Journal, “In 2018, 332 people in Minnesota reported being born in Afghanistan, a number that stayed fairly consistent for several years. But by 2022, that number jumped to 1,107 people.
“The Minnesota Department of Human Services reported that even more Afghans are living in Minnesota than the Census Bureau reports. More than 1,300 evacuees came to Minnesota between September 2021 and September 2022, according to the department.”
Not surprisingly, it’s a tough transition for refugees who have been ripped out of their communities halfway across the world. The Sahan Journal piece details the struggles of individuals and the programming offered by the Afghan Cultural Society. The story is well worth a look for organizations bracing for the next wave of arrivals.
Black Moms: We’re Ignored, Dismissed
 Another entry in the ledger regarding medical treatment of pregnant Black women, courtesy of the New York Times: How Unconscious Bias in Health Care Puts Pregnant Black Women at Higher Risk.
Another entry in the ledger regarding medical treatment of pregnant Black women, courtesy of the New York Times: How Unconscious Bias in Health Care Puts Pregnant Black Women at Higher Risk.
Black women say that too frequently medical providers do not listen when they describe symptoms, or dismiss their concerns. Reports the Times: “Studies validate their experiences: Analyses of taped conversations between physicians and patients have found that doctors dominate the conversation more with Black patients and don’t ask as many questions as they do of white patients. In medical notes, doctors are more likely to express skepticism about the symptoms Black patients report.”
Among the results for Black vs. white mothers are loss of more infants in the first year of life, higher rates of stillbirth and more pre-term births. Differences prevail even when the wealthiest Black women are compared to white women.
Read the complete piece for heart-breaking examples of what transpires when pregnant Black women are ignored, or their concerns get diminished, by white providers.
Posing a Potentially Awkward Question
 Sometimes it’s the little things that can mess you up. Case in point: sensitively asking where your recently-arrived immigrant patient is from or may recently have been. This information allows you to offer country-specific screenings for asymptomatic conditions that can cause health problems later. But depending on immigration status or other factors, it can be a delicate and potentially fraught conversation.
Sometimes it’s the little things that can mess you up. Case in point: sensitively asking where your recently-arrived immigrant patient is from or may recently have been. This information allows you to offer country-specific screenings for asymptomatic conditions that can cause health problems later. But depending on immigration status or other factors, it can be a delicate and potentially fraught conversation.
A guide sheet from Children’s Hospital of Philadelphia offers basic principles and a loose script on how to approach patients. Download the PDF, Ask Where: Communication Guidance for Clinicians Implementing Immigrant Child Health Screening in Primary Care here.
Child Interpreters: The Burden They Carry
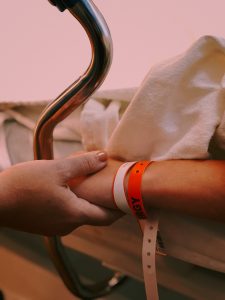 Should you ever think it’s okay to use a child as a medical interpreter for other family members, consider this essay on Multilingual by Onelia Navarro.
Should you ever think it’s okay to use a child as a medical interpreter for other family members, consider this essay on Multilingual by Onelia Navarro.
In it, Navarro recalls a pair of shocking incidents. In one, Navarro was called on to interpret for her parents that she was about to undergo cancer surgery that had a low survival rate. In another, Navarro’s mother picked her up from school to interpret a work meeting that she did not understand. Navarro found herself telling 15 Spanish-speaking workers that they were all about to be fired.
“I was usually praised for being a “mature and helpful” child,” Navarro recalls. “However, people did not realize how stressful this was for me. I was, by then, an 11-year-old kid, and I was constantly struggling due to uncertainty about my ability to deliver messages accurately in both languages. I had to grow up quickly to be able to understand adult life without getting the chance to process the difficult information I was being asked to interpret.”
Read the complete essay for the personal reflection and for a summary on when it might be permissible to use a child to interpret. The short answer to that: “Simply put, children must not be used to provide language assistance to LEP people with only one exception — a life-threatening emergency that requires language interpretation.”
The Disparities File: Unnecessary Amputations
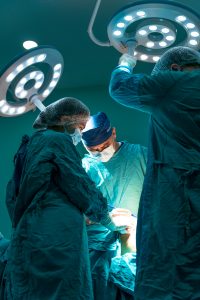 Here’s another addition to the horrifying-instances-of-medical-disparities file. In a recent New York Times opinion piece, My Patient Did Not Have to Die the Way She Did, Dr. Anahita Dua recounts the harrowing case of a Black female complaining of pain in her foot.
Here’s another addition to the horrifying-instances-of-medical-disparities file. In a recent New York Times opinion piece, My Patient Did Not Have to Die the Way She Did, Dr. Anahita Dua recounts the harrowing case of a Black female complaining of pain in her foot.
Dua, co-director of the Massachusetts General Hospital Peripheral Artery Disease Center, recognized the problem as peripheral artery disease. Earlier treatment might have prevented Dua’s remaining course of action: immediate amputation of the infected leg.
Amputation should be a last resort, Dua writes, if routine monitoring and lifestyle changes are part of a treatment plan. But good luck on that if you’re Black. “Black Americans with the disease are less likely to be offered treatment that can restore blood flow, known as limb salvage, compared with white patients,” Dua observes. “Black Americans also pay more for hospitalization costs and have a lower rate of successful limb salvage compared with white patients.”
Writing Systems of the World, Explained
Is it true that Korean is the most scientific writing system, as described by Asian scholar Edwin Reischauer? Get a feel for the various writing systems of the world in the YouTube video above.
The Roman alphabet gets stacked alongside other systems — abjabs, abugidas, syllabaries, and logo-syllabaries — of which most English readers are at best dimly aware. It’s another interesting look at the variety of approaches to the fundamentals of communication.
Race: Not a Predictor for Heart Attack, Stroke
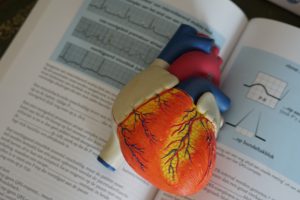 Does race help determine who’s most at risk for heart attack or stroke?
Does race help determine who’s most at risk for heart attack or stroke?
After years of including this factor in its risk assessment tools, the American Heart Association is yanking it from the equation.
In this New York Times story, Race Cannot Be Used to Predict Heart Disease, Scientists Say, Dr. Sadiya Khan observes, “We should not be using race to inform whether someone gets a treatment or doesn’t get a treatment.'” Kahn, a preventive cardiologist at Northwestern University Feinberg School of Medicine, chaired the statement writing committee for the American Heart Association.
This change in keeping with a broader trend in US healthcare that aims at removing race from a variety of clinical algorithms.
Free Covid Test Kits from Site in Multiple Languages
 Sad to say, it’s still handy to have Covid test kits around the house. Here’s a way for your limited English clients to order up a free batch in their first language.
Sad to say, it’s still handy to have Covid test kits around the house. Here’s a way for your limited English clients to order up a free batch in their first language.
Steer them toward this Minnesota Department of Health site, Say Yes! to Covid Test, accessible here. A drop down menu in the upper right corner offers translations in 37 languages plus English.
Rich Set of Resources for Afghan Refugees
 Hoping to understand and work more effectively with recent Afghan refugees? Take a look at this deep collection of respiratory illness-related information and resources available via the University of Minnesota’s National Resource Center for Refugees, Immigrants, and Migrants (NRC-RIM).
Hoping to understand and work more effectively with recent Afghan refugees? Take a look at this deep collection of respiratory illness-related information and resources available via the University of Minnesota’s National Resource Center for Refugees, Immigrants, and Migrants (NRC-RIM).
With more than 88,000 Afghani refugees settled in the US since the 2021 Taliban take-over of the country, NRC-RIM’s guide is a good starting point for improving your work with this new population. The online curated collection, available here, deals with topics including:
Get Covid Videos in ASL
Here’s a trove of colorful ASL videos from the Minnesota Department of Health. The numerous offerings include topics such as:
- Protect Your Child from Covid 19
- Vaccines and Kids
- What Teens Should Know
- What Are Breakthrough Cases?
- What Are Covid 19 Booster Shots”
- And much more
State of the Art: AI and Machine Translation

Wondering how artificial intelligence apps and machine translation will change the landscape for language access? Here’s a free webinar offered by Cross Cultural Communications, set for Wed., Nov. 8, 2023, 10:30 AM.
What Role do AI and MT have in Language Access? will explore AI and MT technologies related to language access in healthcare. Presenters will discuss how these technologies are addressed in Federal laws and regulations, as well as the potential pitfalls associated with their use. Current civil rights complaints, regulatory actions, and peer-reviewed research on language technology and access will underpin the presentation.
Participants will:
- understand the underlying Federal laws and regulations requiring language access,
- understand the uses and limitations of AI and MT,
- be able to articulate the value of human interpreters and translators.
The Pandemic: What MDH Learned about Cultural Communication
 What were the wins, challenges and lessons learned as the Minnesota Department of Public Health’s Refugee and International Health program grappled with the pandemic’s effect on refugee, immigrant and migrant (RIM) populations? Get an assessment at this webinar, Cultural Communications at MDH: Successes, Challenges and Lessons Learned, scheduled for 1-2:30 pm, Wednesday, October 25.
What were the wins, challenges and lessons learned as the Minnesota Department of Public Health’s Refugee and International Health program grappled with the pandemic’s effect on refugee, immigrant and migrant (RIM) populations? Get an assessment at this webinar, Cultural Communications at MDH: Successes, Challenges and Lessons Learned, scheduled for 1-2:30 pm, Wednesday, October 25.
Presenters will share promising practices about embedding cultural communication so public health agencies and other organizations can increase their ability to inform diverse communities and cultures.
By the end of the webinar participants working with RIM communities should be able to:
- define cultural communication.
- understand the principles of embedding cultural communication.
- apply strategies of embedding cultural communication.
Language Access: Learn the Law
 There’s still time to register for a free online training course that explores the laws that govern language access for limited English speakers, scheduled for this Wednesday, October 11, starting at 10 am. The webinar will outline providers’ legal obligations to provide translated and interpreted services, and outine how to respond when those laws are violated.
There’s still time to register for a free online training course that explores the laws that govern language access for limited English speakers, scheduled for this Wednesday, October 11, starting at 10 am. The webinar will outline providers’ legal obligations to provide translated and interpreted services, and outine how to respond when those laws are violated.
The session is offered by Blue Horizon, the online training platform for Cross-Cultural Communications, and will be led by Carol Velandia (right), a University of Maryland Graduate Professor, language access advocate and curriculum developer.
Learn How to Sharpen Online Communication
 Here”s a free class from Yale University that can help you use social and behavioral insights to create, implement and evaluate health communications online.
Here”s a free class from Yale University that can help you use social and behavioral insights to create, implement and evaluate health communications online.
Digital Media for Health Outcomes is designed as an evidence-based tutorial on the key steps to develop successful health campaigns on social media, and to evaluate their performance and impact on health behavior.
Instructors will explore best practices for building messages and campaigns. By the end of the course, you’ll be able to implement a digital communication strategy and evaluate its impact through ad metrics, survey data, cost, and coverage indicators.
Language Barriers Keep Hispanics from Care
 Good news on breaking down language barriers for Hispanic patients? No, not really, according to a survey funded by a supplemental medical insurance provider, Aflac.
Good news on breaking down language barriers for Hispanic patients? No, not really, according to a survey funded by a supplemental medical insurance provider, Aflac.
In the national 2023 study of Spanish-speaking patients, a third of the 2,001 employed adults surveyed said language is an obstacle in their path toward meeting medical needs and understanding insurance policies.
Some key findings include:
- Language Barrier Impact — Language barriers prevent 31% of Hispanics from accessing preventive care resources such as blood tests, pap smears, mammograms, STDs, skin cancer, and colonoscopies.
- Skipping Checkups — The study found that 25% of Hispanics skip regular checkups. Reasons cited include lack of insurance, uncovered costs, and labor disputes.
- Demanding Better Care — More than 60 percent of Hispanic respondents said that healthcare providers and organizations need to better engage and educate the Latino community on the benefits of being proactive with their health and wellness.
- Gender Dynamics — Hispanic men have a more positive outlook on their current and future health compared to women, especially on issues such as controlling their current weight/BMI (64% vs. 45%); financial health (57% vs. 44%); mental health (71% vs. 62%); and physical health (77% vs. 63%).
Seat at the Table: Serve on Equitable Health Care Task Force
 Here’s a chance to voice your opinions on health equity and optimal health outcomes — and in a way that’s more likely to result in change than simply mumbling around the water cooler.
Here’s a chance to voice your opinions on health equity and optimal health outcomes — and in a way that’s more likely to result in change than simply mumbling around the water cooler.
The Minnesota Department of Health is looking for members to sit on its legislatively-mandated Equitable Health Care Task Force. Members will examine race, religion, culture, sexual orientation, gender identity, age and disability as they search for ways to guarantee respectful and equitable care.
Want to apply for a seat? Go to Equitable Health Care Task Force or Board/Commission Equitable Health Care Task Force. Applicants must submit a cover letter; other materials such as resumes and letters of recommendation are optional.
Conference Goal: Make Health Education Material Relevant
 Translating health education materials is a step in the right direction. But if the material is difficult to understand in English, translation won’t make it better. Get insight on improving the usefulness of your communication at the virtual Health Literacy Annual Research Conference, hosted by Health Literacy Research and Practice and scheduled for October 30-31.
Translating health education materials is a step in the right direction. But if the material is difficult to understand in English, translation won’t make it better. Get insight on improving the usefulness of your communication at the virtual Health Literacy Annual Research Conference, hosted by Health Literacy Research and Practice and scheduled for October 30-31.
Keynote Addresses include:
- Making Numbers Meaningful for Patients and Clients, Jessica Ancker PhD, MPH, FACMI, Professor and Vice Chair for Educational Affairs, Department of Biomedical Informatics, Vanderbilt University Medical Center
- The Chatbot Told Me to Stop Taking My Medication – Health Literacy and Large Language Models, Tim Bickmore PhD, MSE, BSE, Professor, Khoury College of Computer Sciences, Northeastern University
<
This online conference includes more than 35 speakers in over two dozen sessions. Among them:
|
Human Interpreters: How threatened by AI?
 What’s does job security look like for interpreters in the face of recent advances in artificial intelligence? Get the low down from Middlebury Institute of International Studies associate professor Barry Olson, a conference interpreter with 25 years of experience. Olson is also the founder of Interpret America.
What’s does job security look like for interpreters in the face of recent advances in artificial intelligence? Get the low down from Middlebury Institute of International Studies associate professor Barry Olson, a conference interpreter with 25 years of experience. Olson is also the founder of Interpret America.
In his in-depth review, Olsen breaks this moment in time into three baskets:
- Technologies for the delivery of interpreting services
- Technologies that augment an interpreter’s performance
- Technologies designed to replace human interpreters‘ purpose altogether
There are situations in which good enough is good enough — where AI more or less gets the job done. But in medical, legal and diplomatic venues, uncorrected mistakes could be catastrophic. Hold on tight as the future of interpreting reveals itself.
Webinar Helps Put Communication in Cultural Context
 Getting the language right in health communication is one thing, but placing the words in a relevant cultural context is another. Get insight from industry experts on creating a culturally appropriate environment in a Public Health Communications Collaborative webinar, Noon – 1:30 pm, Thursday, September 21.
Getting the language right in health communication is one thing, but placing the words in a relevant cultural context is another. Get insight from industry experts on creating a culturally appropriate environment in a Public Health Communications Collaborative webinar, Noon – 1:30 pm, Thursday, September 21.
Panelists include:
- Erica Chung, MPH, COVID-19 Cultural Communications Specialist, Minnesota Department of Health
- Maria Griffin, Owner, Spo-ka’nay Enterprises
- Syreeta Wilkins, Communications Strategist, National Resource Center for Refugees, Immigrants, and Migrants (NRC-RIM)
Zoom registration available at Culturally Driven Strategies: Tailoring Health Communications to Build Understanding and Trust.
Medical Interpretation in the U.S.: Inadequate Approaches Harm Patients
 Here’s a dose of bad news from the Hastings Center on the failures of medical interpretation and the resulting harm to patients.
Here’s a dose of bad news from the Hastings Center on the failures of medical interpretation and the resulting harm to patients.
In this recent essay, Medical Interpretation in the U.S. is Inadequate and Harming Patients, a team of writers observe that there’s a shortage of in-person medical interpreters, which has led hospitals to turn to machine language tools such as Google Translate. You’re more likely to end up in the ballpark if the language in question is Spanish, but watch out if it is, for instance, Chinese. Studies that compare Spanish and Chinese interpretations found that errors are more common in Chinese and more likely to present life-threatening harm.
Throw in a lack of cultural competence training among staff interpreters, and the consequences can include delayed emergency care for children, an increase in errors and costs, and a decrease in care quality and patient satisfaction.
The Hastings Center report goes beyond the mere translation of words and digs deeper into the nuances of the medical exchange. “Expecting patients to adhere to Western constructs of health communication is unfair and unjust,” writers Riya Dahima, Melinda Luo and Vrushali Dhongade contend. “We must consider how linguistic differences and cultural values impact patients’ expectations and decision-making.”
Hazy Days, Health Risks: Info in Spanish, English
 Those hazy days that result from distant fires raise an obvious question: what can I do to protect myself and my family both indoors and outdoors? Here’s information in Spanish and English that offers steps you and your patients can take, plus an explanation on what air quality is and how it is evaluated.
Those hazy days that result from distant fires raise an obvious question: what can I do to protect myself and my family both indoors and outdoors? Here’s information in Spanish and English that offers steps you and your patients can take, plus an explanation on what air quality is and how it is evaluated.
Download this resource from the Public Health Communications Collaborative here.
Stress and Self-Care: Get Tips on How to Cope

Are you or your co-workers worn down by the stress of trying to meet the needs of immigrant and refugee communities? Here’s information that can help, to be offered by the Metro Immigrant and Refugee Health Network in a WebEx meeting scheduled for Tues., Aug. 8, 9:30-11 am.
The program, Self-Care for Professionals Working with Immigrant and Refugee Communities, will be presented by Dr. Christine Danner, Director of Behavioral Health at MHealth Fairview Clinic Bethesda.
Also included in the program is an overview of the voter registration process.
Register here by Aug. 7. After you register, you will receive an email with instructions for joining the meeting online or by phone. Direct questions to cynthia.trevino@state.
Webinar Tackles Traumatic Stress in Refugee Kids
 Among the challenges for refugee youth: overcoming stress resulting from migration and resettlement. At worst they can be subject to abuse, exploitation and trafficking, but also routinely suffer from limited access to resources and the dislocation of existing as a stranger in a strange land.
Among the challenges for refugee youth: overcoming stress resulting from migration and resettlement. At worst they can be subject to abuse, exploitation and trafficking, but also routinely suffer from limited access to resources and the dislocation of existing as a stranger in a strange land.
This free webinar, set for Tuesday, August 1, 12 p.m., will help you define and identify abuse, exploitation and trafficking and offer you strategies for responding. Training is intended for caseworkers, healthcare and mental health professionals, teachers, and anyone else serving children and youth.
Register here: Traumatic Stress Among Refugee Children
Interpreters: Only the Lonely?
 What is a problem all too common for medical interpreters? When Kelly Henriquez asked that question at a panel on interpreter self-care at a national conference, the answer she got was, Loneliness.
What is a problem all too common for medical interpreters? When Kelly Henriquez asked that question at a panel on interpreter self-care at a national conference, the answer she got was, Loneliness.
Henriquez, a dual-certified Spanish medical/healthcare interpreter working in Virginia, noted these trends:
- Many interpreters don’t know where to turn for help.
- Fourteen percent reported they never got training on how to address their mental health needs.
- In-person interpreters were more likely to get an emotional boost from their work.
- Remote workers were more likely to report a decline in mental health.
- Certification such as that offered by the National Board of Certification for Medical Interpreters was a predictor of how many tools interpreters had to fight feelings of isolation and loneliness.
For more detail, and for self-care tips, find Henriquez’s blog post on the subject here.
Taking It to the Next Level: Simultaneous Interpretation
It’s one thing to interpret with pauses allowed in the exchange between speakers. But as this amusing and instructive video explains, simultaneous interpretation is a more daunting and sophisticated task that requires years of preparation.
The instance depicted by the video throws an especially hard curve, in that the interpreted conversation is between earthlings and an alien. Probably not a situation you’ll encounter in your professional role, but well worth a look to expand your knowledge of the interpreter’s job.
The Art Behind Translation
 Usually we’re here concerned with the utilitarian aspects of translation. How does a Hmong patient, for example, best learn more about foot care with diabetes, post-op care or child immunization schedules?
Usually we’re here concerned with the utilitarian aspects of translation. How does a Hmong patient, for example, best learn more about foot care with diabetes, post-op care or child immunization schedules?
This week let’s take a step off the path and consider the artistic aspects of the translator’s job. In this New York Times piece, “Building Something Together’: Translators Discuss Their Art,” five translators describe the joys and frustrations of turning literature from other languages into English.
Literary translators have often gone unrecognized, and the profession has never been much of a route to wealth. Yet, as the Times observes, “The act of carrying a work from one language to another — an art as much as a craft — is anything but mechanical: Translators’ choices are informed by their sensibilities, their emotional landscape, their background.”

 Madeleine Schwartz had what sounds like a complicated but fascinating childhood. She lived with her mother in New York for half the year, and with her father in France for the other six months.
Madeleine Schwartz had what sounds like a complicated but fascinating childhood. She lived with her mother in New York for half the year, and with her father in France for the other six months.